 Biobanks serve as a source of primary human tissues, with some storing millions of samples from hundreds of thousands of patients. So, what do biobanking and COVID-19 have to do with each other?
Biobanks serve as a source of primary human tissues, with some storing millions of samples from hundreds of thousands of patients. So, what do biobanking and COVID-19 have to do with each other?
Genetic marker analysis
These institutions are reservoirs for translational and clinical research, providing human samples that can be tested for genetic markers related to specific diseases. Infection with SARS-CoV-2 appears to have a widely heterogenous outcome, ranging anywhere from asymptomatic carrier to fatal disease. Though most fatalities are older patients and there is a link between obesity, diabetes, and hypertension with increased disease severity, there is no clear-cut reason why the disease appears to affect certain healthy patients with no major health issues and not others. Data garnered from biobanks can help solve this mystery by identifying specific traits that may correlate with a higher risk for severe disease, potentially leading to a better understanding of the virus and more targeted therapies.
A Quebec biobank leads the way
Quebec has no doubt been hit the hardest in Canada, accounting for around half of all cases and fatalities in the country. It’s no surprise then that two of the early leaders in biobank development for COVID-19 are the Fonds de recherche du Québec (FRQ) and Genome Québec, who began operating the Québec COVID-19 Biobank in April. Led by McGill’s Dr. Vincent Mooser, the biobank will collect samples and data from infected individuals and create a network for many of the major Quebec universities to participate in COVID-19-related research. Included in the task force that will run the biobank are members from Université de Montreal, McGill University, the McGill University Health Centre, and the Fonds de recherche du Québec – Santé (FRQS). These members will coordinate the use of the existing infrastructure like the biobank of the Quebec Respiratory Health Research Network (Réseau de Recherche en Santé Respiratoire du Québec (RSRQ) and population-based cohort databases, such as CARTaGENE and the Canadian Longitudinal Study on Aging (CLSA).1
Biogen chips in after “superspreader” event
Another consortium with high-profile members, such as Harvard University, Biogen Inc., Partners Healthcare, and MIT is set to build a COVID-19 biobank in the United States. Notably, those who were infected at a management meeting hosted by Biogen in February thought to be a “superspreader” event that led to the initial uptick in cases throughout Massachusetts, are eligible to be the first patients to have samples collected by the biobank, once it’s up and running.2 The Biogen event is notable as it was one of the first instances in the United States where a large group of people were responsible for unknowingly becoming infected at a meeting and later traveling across the country, unaware that they were to infect others. In three states (North Carolina, Indiana, and Tennessee), they were the first known transmitters of the virus.3
The UK Biobank provides existing infrastructure in Europe
The UK Biobank is one of the largest biobanks worldwide, with medical information and patient samples from 500,000 participants whose health has been tracked for the last ten years. The biobank was initially set up to study a variety of diseases, ranging from cancer to Alzheimer’s disease. However, it is now placing COVID-19 front and center as it publishes every week both positive and negative SARS-CoV-2 test results from many of its participants. It also plans to make the following data available to researchers: primary care data, hospital inpatient data, deaths, and critical care data for participants with confirmed COVID-19.4
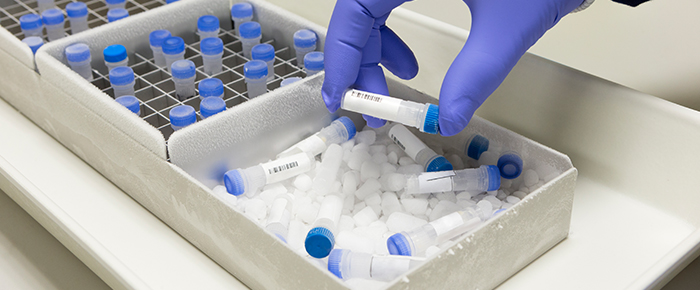
Biobanking and COVID-19 patient specimens
Biosafety is key when dealing with human specimens, particularly those derived from patients with COVID-19, as any leak can expose personnel to the deadly virus. On February 12, 2020, the World Health Organization released guidelines for handling these specimens.5 Important in their assessment is that any procedure must minimize the risk of droplets or aerosols that can potentially lead to airborne propagation of the virus. Furthermore, appropriate personal protective equipment is necessary based on a thorough risk assessment. This risk assessment should ideally cover every step of specimen handling, from isolation to processing.
Generally, handling of high concentrations of the virus, including viral propagation, require a BSL-3 containment facility, whereas procedures involving potentially infectious material (e.g. extracting RNA, DNA, or proteins from infected tissue) require handling under a biosafety cabinet or using another similar protective device. Airflow is another factor to consider, as it’s recommended to use a controlled ventilation system that provides inward directional airflow into the lab and prevents exhaust air (which must be HEPA filtered) from reaching other areas of the building.
When packaging and shipping samples, any containers that contain the virus should be placed in a secondary container, minimizing the potential for spills. Naturally, all containers need to be appropriately labeled: patient specimens from suspected or confirmed cases are identified as UN3373, “Biological Substance Category B” whereas viral cultures or isolates need to be identified as Category A UN2814, “infectious substance, affecting humans.”
LabTAG by GA International is a leading manufacturer of high-performance specialty labels and a supplier of identification solutions used in research and medical labs as well as healthcare institutions.
References:
- Nishihata J. FRQ to create a province-wide COVID-19 Biobank. McGill REPORTER. https://reporter.mcgill.ca/frq-to-create-a-province-wide-covid-19-biobank/. Published 2020.
- Biogen. Building a COVID-19 Biobank: A new consortium led by Biogen and The Broad Institute of MIT and Harvard. https://www.biogen.com/en_us/covid-19-updates/biobank.html. Published 2020.
- Stockman F, Barker K. How a Premier U.S. Drug Company Became a Virus ‘Super Spreader.’ The New York Times. April 12, 2020.
- UK Biobank. UK Biobank Makes Infection and Health Data Available to Tackle COVID-19. https://www.ukbiobank.ac.uk/2020/04/covid/. Published 2020.
- World Health Organization. Laboratory Biosafety Guidance Related to Coronavirus Disease 2019 (COVID-19). Geneva, Switzerland; 2020.